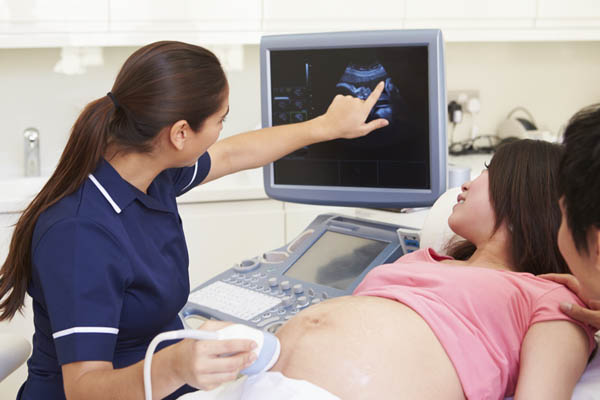
When people think of ultrasound, oftentimes obstetric ultrasound is the first thing to come to mind. For many, it is the very reason they begin to explore the profession of being an ultrasound technologist in the first place! Sonographers have the unique experience of playing a role in a mother’s pregnancy.
These highly skilled healthcare professionals have the responsibility of obtaining images for physicians to monitor a baby during development. Sonographers are often the first to see many of the exciting moments in a pregnancy—the heartbeat, movement, twins, the sex of the baby, etc.
If you are here to explore a potential career as an obstetric sonographer, continue reading to familiarize yourself with the career path process.
How do you Become an Ob/Gyn Sonographer?
Sonographers must undergo formal education and training to gain foundational knowledge and skills to practice as an ultrasound technologist. Typically, a two-year Associate or four-year Bachelor’s degree is completed at an accredited institution of higher education such as a community college or university.
It’s very important to find the right program to suit your educational needs. Find a reputable program that has proven its excellence through program accreditation, not just college or university level accreditation. To find a school accredited by CAAHEP (Commission on Accreditation of Allied Health Education Programs), start here at https://www.caahep.org/Students/Find-a-Program.aspx.
A great career as any healthcare professional starts with a great education… doing your research will help you be confident that your time and money is being spent in a worthwhile place.
Prerequisites for Applying to an Ultrasound Program
Now that you know you want to be a sonographer and where you may like to learn the skills to become one, you must complete the necessary prerequisite coursework to apply to a program. Most sonography programs require an admission process separate from the sponsoring institution. For example, you may complete a year and a half of prerequisites and then two years of coursework specific to sonography.
Common prerequisite coursework for sonography programs include: anatomy and physiology, physics, college algebra, English, medical terminology, and psychology. Your academic advisor is going to be your new best friend!
Complete Your Ultrasound Degree
Once you enter your sonography program you will typically complete courses in cross sectional anatomy, sonographic physics and instrumentation, and patient care. You will complete didactic, laboratory, and clinical coursework in the specialty areas your specific program teaches.
- Didactic courses present information about anatomy, physiology, and pathophysiology that you encounter in a clinical setting.
- Laboratory courses give you an opportunity to practice and break down scanning techniques sonographers use to acquire reliable, diagnostic images on volunteer scan models or other simulation-based environments.
- Clinical courses are designed to give students experiential hours in various sonography settings. Rotations may include clinical time in hospitals, outpatient centers, and physician offices. Students often rotate through various departments to get a well-rounded experience and feel for the professional work environment. Clinical courses are the place to build the skillset to demonstrate competency and proficiency in the performance of sonographic examinations, caring for patients, and working as a member of the healthcare team.
Obtain Your RDMS Credentials
It is highly likely that any potential employer will require you to have your RDMS credential.
The Registered Diagnostic Medical Sonographer (RDMS) credential is awarded by the American Registry for Diagnostic Medical Sonography to applicants that have completed the necessary didactic and practical experience and successfully pass 1) the sonographic physics and instrumentation examination
and 2) the obstetric and gynecology specialty exam.
To maintain the RDMS credential and good standing with the ARDMS, 30 continuing medical education (CME) credits are required every 3 years. An annual membership fee is also required. Sonographers often obtain these CME requirements through clinical instructorship of students in CAAHEP-accredited programs, attending virtual or live conferences, ultrasound applications training from vendors, reading peer-reviewed sonography journals, or even publishing their own case studies and research.
Obstetric Sonographer Job Requirements
All sonographers must possess the ability to perform a highly technical skill with a compassionate delivery. Being an obstetric patient can be a happy and exciting time in a mother’s life, but it can come with worrisome and sad moments. It is important for a sonographer wanting to work in obstetrics/gynecology to understand that they will be caring for patients under stress and worry alongside happiness and excitement.
Where do OB Sonographers Work?
Many prospective sonography students are attracted to the idea of working in an OB/GYN office. However, there are many diverse opportunities for work environments in the OB/GYN specialty:
- Inpatient
- Outpatient
- Stand alone imaging facilities
- Travel/contract
The sonography profession (like most healthcare professions) has staffing needs during days, evenings, nights, holidays, weekends, and often requires call coverage depending on the employer’s needs. It is important to understand that outpatient, day shift positions are often competitive and are a fast-paced
environment. Sonographers that are new to the profession may need to work in various settings to gain paid work experience for a robust resume.
Learn More About Obstetric Ultrasound
Common Indications for OB/GYN Examinations
There are many different reasons a physician may order an ultrasound to be performed by a sonographer! An indication is the reason a study is being performed. For example, a physician may order a pelvic ultrasound to evaluate post-menopausal bleeding in a 64-year-old woman.
Indications for Gynecologic Ultrasound
– Pelvic pain
– Abnormal menstrual cycles
– Missed menstrual cycle
– Post-menopausal bleeding
– Ovarian cysts
– Uterine fibroids
– Intrauterine device placement and/or follow up evaluation
– Ultrasound guidance for other minimally-invasive procedures
Indications for Obstetric Ultrasound
– Pregnancy dating
– Evaluation of fetal anatomy
– Evaluation of fetal growth
– Evaluation of fetal well-being
– Bleeding in pregnancy
– Pelvic pain in pregnancy
– Premature rupture of amniotic fluid
– Evaluation of fetal position
Maternal Fetal Medicine (Perinatology)
Maternal fetal medicine (also called perinatology) is a subspecialty of obstetrics. The MFM specialty takes care of high-risk pregnancies. A pregnancy can be considered at a higher-risk because of either a maternal or fetal issue (or both!) hence the name maternal-fetal medicine. Obstetric sonographers may choose to further specialize and work in the perinatology setting. They often perform many of the duties listed previously as well as advanced studies that help maternal-fetal medicine physicians (perinatologists) and obstetricians co-manage pregnancies.
Currently there is no ARDMS certification for perinatology, however, many MFM sonographers must complete additional training and education to become certified to perform fetal echocardiograms (fetal heart studies). Perinatal sonographers may also assist with imaging during procedures such as chorionic villus sampling, amniocentesis, percutaneous umbilical blood sampling (PUBS), and other procedures during the perinatal period.
From the Experts: Interviews with Diagnostic Medical Sonographers:
Chelsey Wright,BS-MIRS, RDCS (AE, PE), RDMS. Learn more about ectopic pregnancies and the implications for mother and baby, and the role that the sonographer plays in diagnosing them.
Stephanie Eisler, RDMS. Stephanie Eisler, Sonographer, RDMS, shares her story of personal fears and triumphs, and how she turned them into a fulfilling career of which she can say her heart is truly in it.